-Feb-16-2021-06-45-35-25-PM.png?width=1080&name=Title_%20How%20to%20Study%20Efficiently%20for%20Hours%20On%20End%20(With%20the%20Help%20of%20a%20Tomato)-Feb-16-2021-06-45-35-25-PM.png) The female reproductive system can at times feel like a difficult jumble of hormones that all seem to be related, but fluctuate in unpredictable ways. To make sense of the particularities of the female reproductive system, especially for exams like the MCAT, it is important to not only know what hormones are involved, but also to understand what their purpose is and how that purpose is connected to their seemingly random (but actually quite predictable!) cyclic fluctuations. Once you know all that, the reproductive system transforms from a confusing jumble of terms to a beautiful concert of hormones working together to drive and maintain the complex processes of ovulation, menstruation, and pregnancy.
The female reproductive system can at times feel like a difficult jumble of hormones that all seem to be related, but fluctuate in unpredictable ways. To make sense of the particularities of the female reproductive system, especially for exams like the MCAT, it is important to not only know what hormones are involved, but also to understand what their purpose is and how that purpose is connected to their seemingly random (but actually quite predictable!) cyclic fluctuations. Once you know all that, the reproductive system transforms from a confusing jumble of terms to a beautiful concert of hormones working together to drive and maintain the complex processes of ovulation, menstruation, and pregnancy.
The Hormones
Before we get started, it is important to introduce the key hormonal players that we will be tracking.
- Progesterone: Important for developing and maintaining the endometrium, a mucous membrane lining the uterus that is the site of implantation by a developing zygote (future fetus).
- Estrogen: Important for general female reproductive system maintenance, including thickening of the endometrium.
- Follicle stimulating hormone (FSH): Stimulates germ cell maturation and promotes estrogen production. Secreted by the anterior pituitary.
- Luteinizing hormone (LH): Promotes progesterone production. Secreted by the anterior pituitary.
- Gonadotropin-releasing hormone (GnRH): Released by the hypothalamus to stimulate FSH and LH production, but not as directly involved in the reproductive cycle signaling as the other hormones listed.
The Menstrual Cycle
Now that we have a sense of the key hormones, let us begin by looking at the menstrual cycle and how its stages relate to the hormones we have outlined. The menstrual cycle is a 28-day cycle that involves building up and developing the endometrium, releasing an egg that may or may not be fertilized by a sperm, and then shedding the endometrium if there is no fertilization and implantation (i.e. no pregnancy). If there is pregnancy, the endometrium needs to be maintained to support the developing fetus. Many of the hormonal fluctuations in the reproductive system make sense when you think about them in relation to the endometrium.
Fun fact: humans are not the only animals that menstruate! Close relatives to humans, like apes and monkeys, as well as a couple other animals (elephant shrews and some bats) undergo the same cycle. Other animals undergo what is called an estrous cycle, which typically occurs for their entire lives.
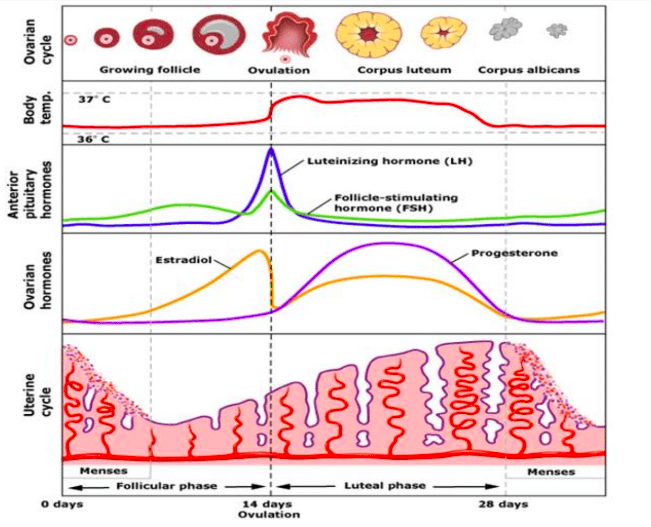
Figure 1: Stages of the menstrual cycle and associated hormonal changes
Follicular phase
The menstrual cycle begins at the follicular phase, which starts on the first day of menstrual flow (endometrial shedding). The follicular phase begins with all the aforementioned hormones expressed at low levels. The hypothalamus (a portion of the brain that is important for endocrine system function) senses these low levels of estrogen and progesterone and secretes GnRH, which increases secretion of FSH (and slightly LH) by the anterior pituitary. FSH, as the follicle stimulating hormone, stimulates progressive maturation of the ovarian follicle (home of the egg). The developing ovarian follicle produces estrogen, which starts to increase dramatically. These increasing levels of estrogen will begin preparing the endometrium again for implantation.
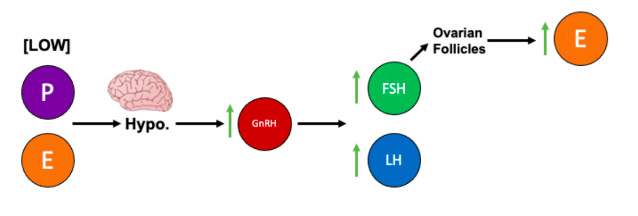
Figure 2: Hormonal changes during the follicular phase. P = progesterone; E = estrogen; Hypo. = hypothalamus.
Ovulation
Towards the end of the follicular phase, the very high levels of estrogen cause FSH and LH to spike, as can be seen in the chart above. At this point, ovulation occurs, which is when the egg pops out of the ovarian follicle due to the spike in LH. As a result of ovulation, the corpus luteum forms. This all makes sense when you think about it: ovulation and the corpus luteum that forms as a result are driven by an increase in LH, the luteinizing hormone.
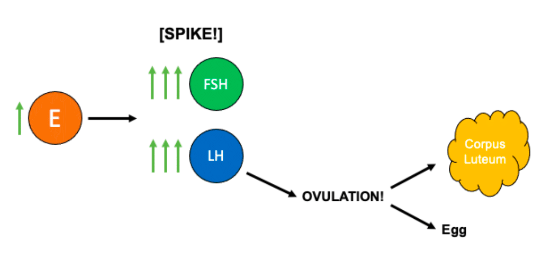
Figure 3: Hormonal changes during ovulation.
Luteal phase
Ovulation releases the egg and leaves behind the corpus luteum. This corpus luteum is now responsible for producing progesterone (see in Figure 1 how progesterone increases after ovulation), which, as we have discussed, further develops and maintains the endometrium for implantation. Importantly, there is also a negative feedback loop between progesterone and LH that will cause LH levels to dip. If no implantation occurs, the corpus luteum will degenerate (LH is necessary to maintain the corpus luteum). Progesterone will then decline (no corpus luteum around to produce it), as will estrogen. The decrease in progesterone and estrogen will cause the endometrium to shed, leading to menstruation.
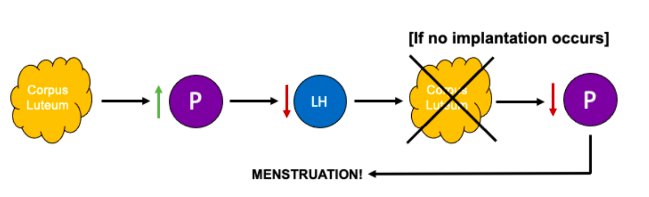
Figure 4: Hormonal changes during the luteal phase.
Pregnancy
All this talk of endometrium preparation begs the following question: what happens when fertilization and implantation do occur?
Recall that progesterone is important for maintaining the endometrium, which is critically important for implantation. Thus, it should make sense that, in order to have a successful pregnancy, you would want to maintain the thing that produces progesterone: the corpus luteum! And this is what happens: if implantation occurs, the implanted blastocyst (you might recall from previous learning that the blastocyst forms around day 5 of development) will produce hCG. hCG is an LH analog that maintains the corpus luteum after LH levels decrease so that the corpus luteum can continue secreting progesterone throughout the first trimester. After the first trimester, the placenta will take over progesterone secretion for the remainder of the pregnancy.
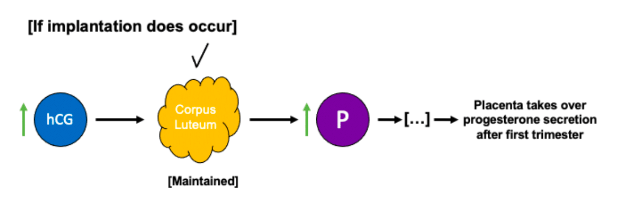
Figure 5: Hormonal changes during pregnancy.
So that is it! Hopefully, you have seen that the female reproductive system is actually quite straightforward when you pay closer attention to how the hormones involved work together to achieve a common purpose: a constant cycle of building and shedding the endometrium on the off chance of one day being home to a developing fetus.
Comments